How the integration of health and disaster risk reduction can set Asia-Pacific on a path towards resilience
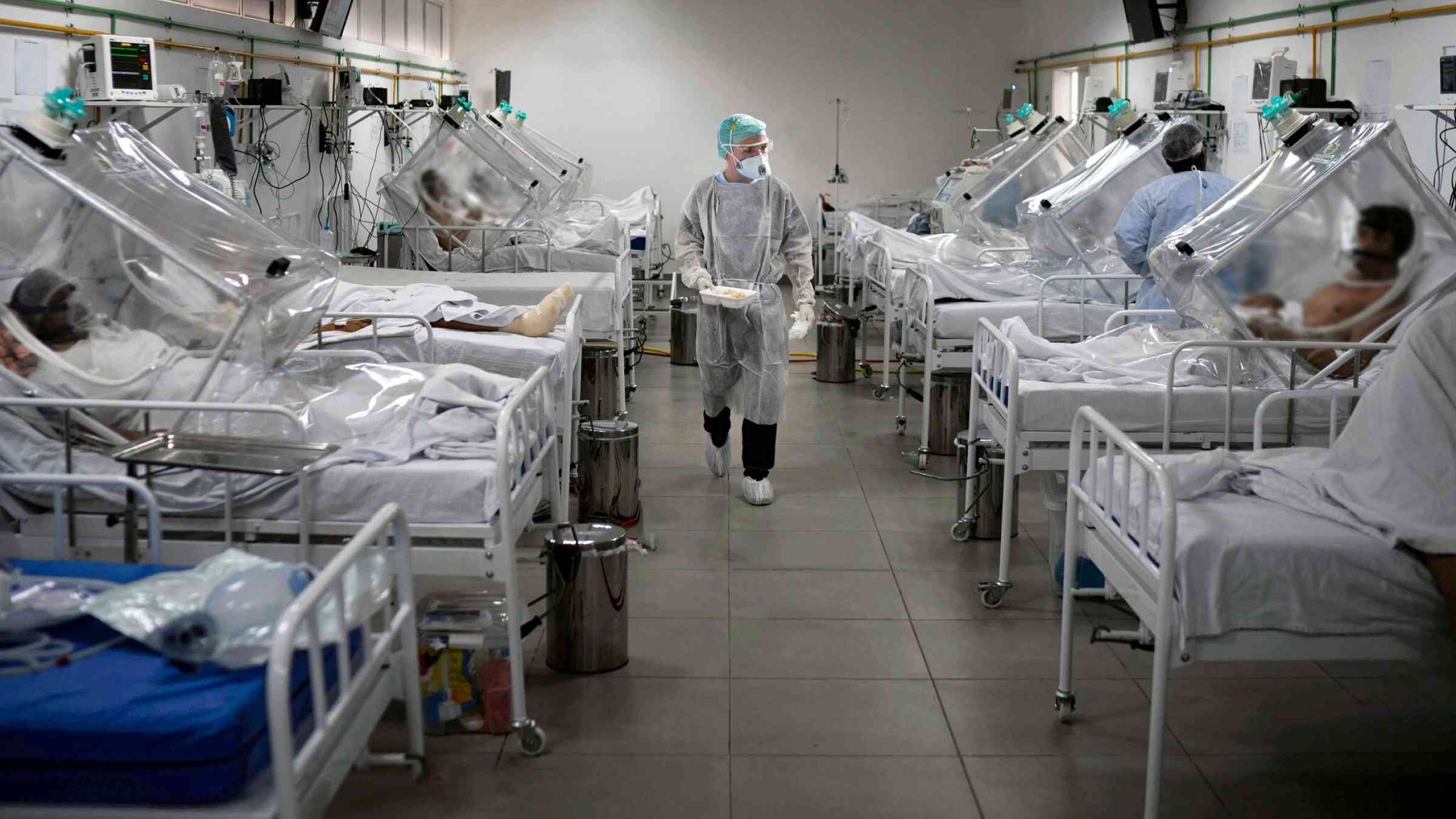
The COVID-19 pandemic was in many an unexpected event that caught the world off guard. The World Economic Forum’s 2020 Global Risks Report, for example, did not include pandemics in its list of 10 most likely risks.
However, while the pandemic was unexpected, it was not unavoidable.
A number of global framework and guidelines were developed in recent years to prevent and manage the occurrence of such disasters.
Key among them is the Sendai Framework for Disaster Risk Reduction 2015-2030, which includes biological hazards, such as pandemics, as one of the main risks that countries ought to plan against in line with the International Health Regulations (2005).
This was followed by the development of the Bangkok Principles in 2016, which call for strengthening the integration between the disaster and health management sectors, and in 2019, the release of the World Health Organization’s (WHO) Health Emergency and Disaster Risk Management (EDRM) Framework.
The COVID-19 pandemic demonstrated a need to ensure that the policy recommendations of these frameworks are followed by countries to both effectively deal with the ongoing crisis and minimize the possibility and impact of a future one.
To facilitate this and to encourage the exchange of lessons from cross-sectoral collaborations in the context of COVID-19, the Asia-Pacific Regional Office of the UN Office for Disaster Risk Reduction and the WHO South-East Asia Regional Office organized a webinar, on 24 February, directed at health and disaster risk reduction focal points across the region.
The webinar, which saw the participation of 473 people, in part of a series of joint efforts between UNDRR and WHO since the onset of the pandemic to strengthen the links between disaster risk reduction and public health.
“We need to sustain this collaboration during COVID-19 and then build on it for concurrent risks of all types of emergencies and disasters, during the pandemic and beyond, and to apply the lessons of the pandemic in our future DRR agenda,” said Dr. Qudsia Huda, Head of Disaster Risk Management and Resilience at WHO headquarters in Geneva, adding:
“WHO is increasing its focus on a risk management and whole-of-society approach. We have learned from the disaster risk management sector that measures to reduce hazards, exposures and vulnerabilities are key.”
This call for cross-sectoral collaboration between health and disaster risk reduction agencies was echoed by UNDRR’s regional Officer-in-Charge, Mr. Animesh Kumar:
“Pandemics after all are a form of disaster. And as it is important that countries establish protocols between agencies and early warning systems to detect natural hazards, such as cyclones and tsunamis, it is equally important that similar efforts and investments be made to reduce the risk of biological hazards and prevent outbreaks from becoming full-blown disasters.”
Countries stand a much better chance at preventing and mitigating pandemics, and other health emergencies, if they adopt a multi-hazard and multi-sectoral approach in how they govern disaster risk.
However, as it stands, many countries have yet to embrace a more expansive view of risks to include all types of hazards, especially biological ones.
“Most national DRR strategies still do not reflect biological hazards and health emergencies into their planning efforts in any great detail,” noted Mr. Timothy Wilcox, Programme Management Officer with UNDRR’s Regional Office for Asia-Pacific, citing a recent UNDRR review that examined COVID-19 disaster risk governance in the region.
Mr. Wilcox offered recommendations on how integration between disaster risk reduction and the health sector could be strengthened, such as offering joint training for disaster and health officials, enhancing data sharing between sectors, and providing technical assistance for the incorporation of health emergencies into national disaster risk reduction strategies and plans.
“Currently there are different sectors with specific plans which need to be interacting with each other through an integrated risk management approach,” said Dr. Anil Bhola, a consultant with WHO South-East Asia Regional Office, who presented an overview of the Health EDRM Framework and voiced his support for integrated planning.
Providing an operational perspective were officials from India, the Maldives, Thailand, Mongolia and the Association of Southeast Asian Nations (ASEAN) Secretariat, who offered their lessons and recommendations on how countries could better position themselves to address health emergencies.
“There are a lot of lessons we have learned, which we will need to hardwire into our national system of preparedness for pandemics and other emergencies,” said Mr. Kamal Kishore, Member of India’s National Disaster Management Authority.
One priority that countries need to address, according to Mr. Kishore, is scalability in response to large or prolonged disasters:
“How do you scale your capacities when you're struck by a pandemic? That really requires a great deal of preparedness.”
One key issue that a number of officials mentioned was the importance of political support to facilitate cross-sectoral integration. This could be in the form of passing new laws that mandate better integration or through executive action by the head of state.
In the case of Mongolia, the parliament amended the ‘Law on Disaster Protection’ and passed a temporary law specific to the prevention of COVID-19 and the mitigation of its social-economic impacts, according to Ms. Bazarragchaa Duudgai, a Senior Specialist with Mongolia’s National Emergency Management Agency.
In the Maldives, the country was able to mobilize its resources for an effective response two months before the first case of community transmission due to presidential support and the flexibility of its existing disaster and health laws.
“In Maldives, elements of the Disaster Management Law was used with the Public Health Regulations. The Disaster Management Law was used to build national capacities and coordination while health regulations were used to deliver critical emergency healthcare,” explained Mr. Hisan Hassan, Chief Executive of the Maldives National Disaster Management Authority.
Beyond the delegation of authority, the clarification of roles and responsibilities was identified as an enabler to enhance collaboration across agencies and sectors.
In the case of Thailand, the country’s Department of Disaster Prevention and Mitigation (DDPM) was not the lead agency for the COVID-19 response but it had a clear understanding of its role, which helped it effectively support the larger effort.
“The Prime Minister divided the tasks between different ministries very clearly,” said Ms. Pannapa Na Nan, Director of the International Cooperation Section at the DDPM, adding:
“DDPM is part of the Ministry of Interior which assumed a supporting role in implementing the measures that were issued by the Ministry of Public Health at the local provincial level and the community level.”
Several also cited the collection of data and analysis of risk information as critical to informing prevention and response efforts, especially to reach the most vulnerable, such as migrant workers and persons with disabilities.
“Maldives rapidly developed a data management system to collect and share data in real-time. The data was used in policy discussions to take decisions,” said Mr. Hassan.
Another issue that several highlighted as a priority was the need for effective risk communication, which is a component of both disaster risk and public health management.
“In combining DRR and public health to prevent a complex situation, crisis communication needs to be conducted very professionally to gain the trust of the people,” noted Ms. Na Nan.
At the regional level, ASEAN has taken a leading role in shaping Southeast Asia’s approach through its multilateral policy tools. Speaking on behalf of the ASEAN Secretariat, Dr. Riyanti Djalante, Assistant Director for Disaster Management and Humanitarian Assistance, asserted that:
“A coherent approach on health and disaster risk management, multi-hazards considerations in disaster risk reduction, and integrated COVID-19 pandemic responses are the key factors” in how ASEAN has responded to the pandemic.
A clear example of this was the adoption of a multi-hazard approach to risk reduction in the 2021-2025 Work Programme for the ASEAN Agreement on Disaster Management and Emergency Response (AADMER).
This shift is in line with UNDRR’s recommendation that disaster risk governance models shift from a reactive hazard-by-hazard approach to an anticipatory system-wide approach, as noted by Mr. Kumar:
“That is what our ultimate goal should be – a state of disaster risk governance that is multi-hazard in scope and multi-sectoral in its composition. It can and should start with better integration with the health sector, but it should not stop there.”